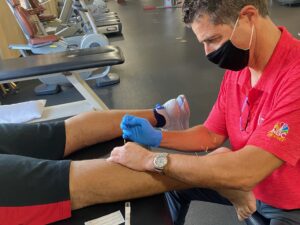
Post-operative state
Surgery is a medical procedure used to treat a problem or, repair or modify some part of the body for better functioning and appearance. It is an intense measure as it requires cutting open the skin and multiple layers of muscles, which are then joined through stitches. Proper reunion of the incision happens after weeks and multiple stages of skin regrowth. Weakness and exhaustion are natural in this period of pain and discomfort. However, proper care post surgery can ensure a speedy and better recovery.
Post-operative physical therapy care has multiple aspects such as wound care to prevent infection, protection from injury, as well as careful movements to enhance the healing.
Importance of physical therapy rehabilitation
Scar formation is a part of healing. In an immobilized area, the scar tissue will have random fibers with no proper arrangement. With early mobility, the gentle pull induces the formation of parallel arranged muscle fibers that are more flexible than the irregular ones.
When scar tissues are contracted, they are highly prone to forming adhesions, which affects the muscle function.
In addition, muscles lose 3 grades of strength post-surgery. Therefore, to regain the lost strength, and to avoid the adhesions from long period of immobility, post-surgical physical therapy becomes an essential component of the rehabilitation process.
Passive range of motion exercises are started early after the surgery within a pain free limit for ideal scar tissue management. Moving on to active and then resistive exercises once the skin has joined completely. Light stretches to skin along the incision line are helpful in reducing the contracture, while the exercises prevent adhesions between the layers of muscles.
- Musculoskeletal surgery, especially when involving joints, are subjected to continuous passive movement within 48 hours. This is crucial for synovial fluid flow and contracture prevention.
- Post neurological surgery rehabilitation involves testing of reflexes and coordination, and exercises to improve coordination. Neurological physical rehabilitation follows a proper sequence similar to the developmental milestones in childhood because the brain has the memory and hence learns faster.
Pain and discomfort can lead to adaptation of abnormal movement patterns, which can continue even after full recovery and cause further problems with posture and alignment, which is why supervised rehabilitation must be continued until the patient has healed.
Bed rest, on the other hand, endangers a person to bed sores, deep venous thrombosis, and continual loss of strength. In contrast, early mobility after surgery enhances the blood flow to the area of incision and promotes healing. Any therapy works best if the patient themselves has a positive outlook. Counseling before and after surgery is helpful in this aspect. Patient motivation and compliance ensures a much faster recovery.